Science continues to explain what we’ve known for a long time. Mothers should eat in a healthy manner while pregnant!
This past week, a study out of Germany was published explaining how for some, the root cause of Type 2 Diabetes might be in the expression of a single gene, and that this gene can be “edited” early in life. A Science Alert story covering this research explained the conclusion:
Intriguingly, researchers had found evidence that the binding protein’s gene had been silenced by an epigenetic switch – the DNA equivalent of a padlock that can be put in place for various reasons, typically environmental ones.
Their findings suggested that the gene for IGFBP-2 in the liver was edited early in life, setting the mice up for type 2 diabetes later.
The field is called epigenetics. The Guardian wrote a very approachable piece on the topic. In it they explain:
Studies of humans whose ancestors survived through periods of starvation in Sweden and the Netherlands suggest that the effects of famine on epigenetics and health can pass through at least three generations. Nutrient deprivation in a recent ancestor seems to prime the body for diabetes and cardiovascular problems, a response that may have evolved to mitigate the effects of any future famines in the same geographic area.
While most popular theories suggest that chronic diseases are caused by genetic factors and lifestyle, scientists now understand that environmental factors are also at play — and not just over long periods of time. Your mother’s nutrition during pregnancy plays a big role in your adult health and risk of Type 2 diabetes and metabolic syndrome.
This theory started with Barker’s hypothesis of 1992. The Oregon Health Sciences University (OHSU) summed up David Barker’s work well.
Over twenty-five years ago, he [David Barker] was the first to show that people who had low birth weight are at greater risk of developing coronary heart disease and diabetes – now a widely accepted fact. This finding led to a new understanding that chronic adult diseases are “programmed” in the womb by malnutrition and other harmful influences.
A decade later, the World Health Organization published a piece called “Programming of chronic disease by impaired fetal nutrition: Evidence and implications for policy and intervention strategies” calling for further research. The New Yorker also wrote a much more approachable piece called 2007 called “Small and Thin” about this topic, which was still considered controversial even by 2007.
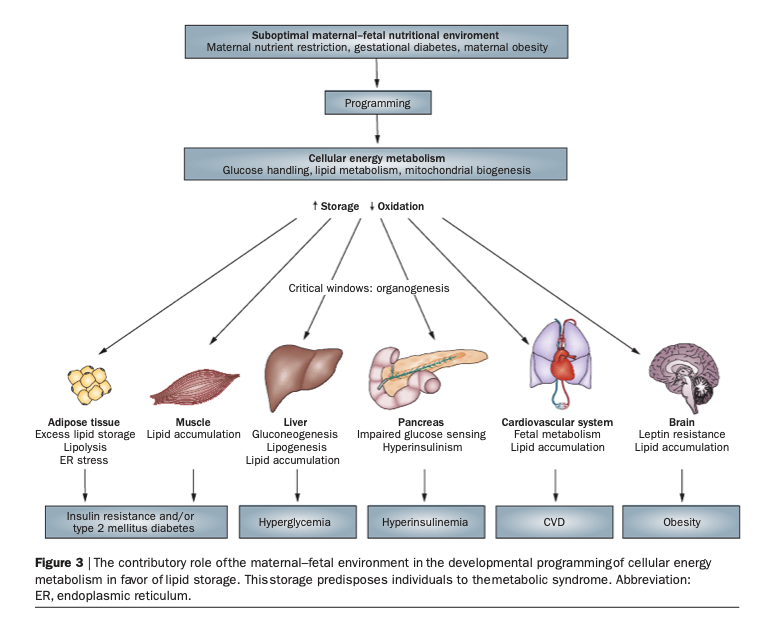
Still, scientific evidence on the impact of epigenetics continues to mount. A literature review of the research was just done in August 2018 called “Nutritional programming of the metabolic syndrome.” In it, they draw an interesting diagram of epigenetic effects of “sub-optimal maternal fed nutritional environments.” (Don’t you love scientists? 😇)
I personally became very interested in this topic back when I found out I had diabetes back in 2003, as I believe that I was personally impacted by epigenetics. While I am not from an impoverished region, my mom — who is known among friends and family to always look her best — only gained 10 pounds when she was pregnant with me. She had boasted to me once that no one even knew she is pregnant until she was 8 months in! The graph below shows that, even for her, she was grossly underweight.

Source: babycenter.com
To sum it up, I think her dieting during pregnancy may have epigenetically impacted my gene for IGBF-2! Of course, there’s a lot we didn’t know back then, and knowing this now doesn’t help me much personally for now. I will still continue my own care as I have been!
Still, for any of you out there who are pregnant or know someone who is, make sure they know to eat well during pregnancy!
Photo by Leah Kelley from Pexels